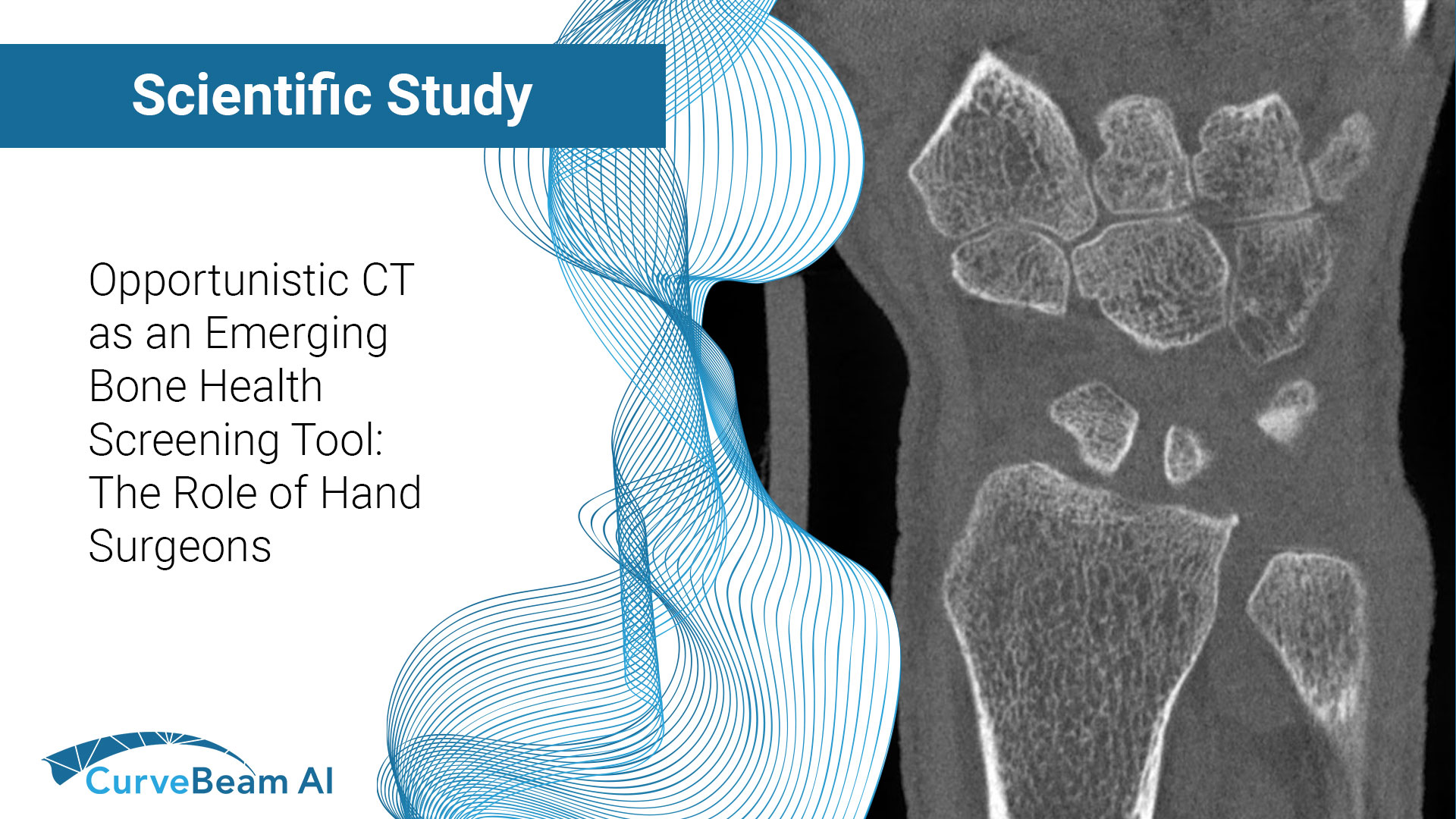
AI-Driven Segmentation on Weight Bearing CT Introduction Accurate segmentation is critical for orthopedic workflows, including…
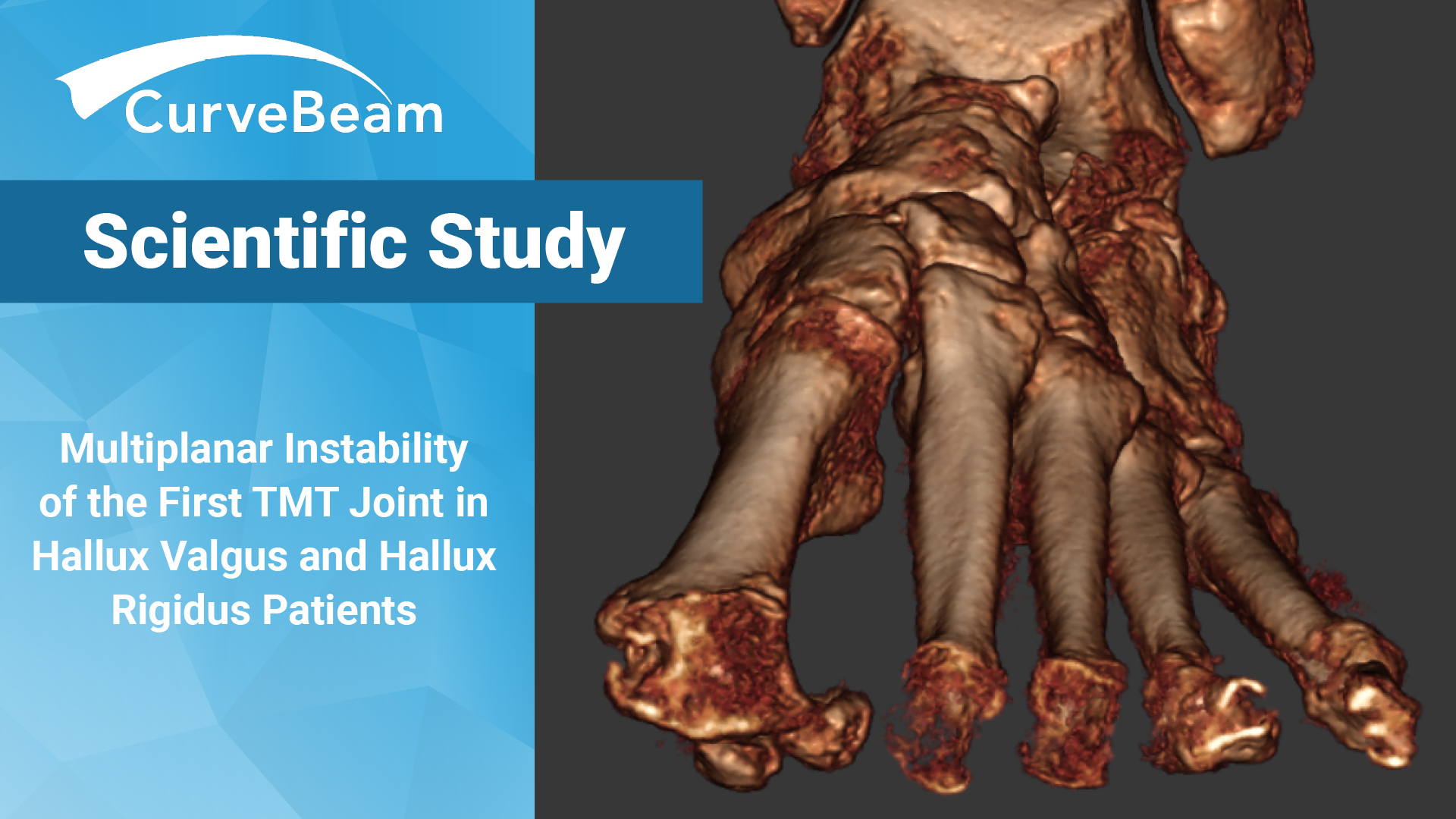
WBCT Confirms 1st TMT Instability in HV & HR Patients
Key Points
- Compared to controls, WBCT scans of hallux valgus (HV) & hallux rigidus (HR) patients confirmed signs of first ray instability at the TMT joint are often present.
- Dorsal translation of the M1 and plantar gapping were other common pathological features on WBCT scans of HV and HR patients.
- The same scans showed C1 morphology is likely not a predisposing factor for first ray instability in HV and HR patients.
1st TMT Instability – Does it Cause Forefoot Pathologies?
Hypermobility of the first ray has been considered closely associated with various forefoot diseases including Hallux Valgus (HV) and Hallux Rigidus (HR). Instability of the first tarsometatarsal (TMT) joint has been described to be associated with development of HV and post-operative HV recurrence. However, numerous researchers suggest that sagittal instability of the first TMT could be the result of HV, not the cause.
Researchers at the University of Iowa Department of Orthopaedics confirmed HV and HR patients have significant multiplanar instability compared to controls using Weight Bearing CT (WBCT) imaging. Their findings were published in the July 2021 issue of International Orthopaedics.
Clinical examinations of hypermobility are limited and have low reliability, while weight bearing conventional radiographs (WBCR) are limited by varying positions of the foot with respect to X-Ray projection and its inability to assess the coronal plane accurately. WBCT is a new and highly reliable and accurate tool that allows for a quantifiable analysis of the first ray hypermobility including multi-planar assessment in axial, sagittal, and coronal planes.
The primary objective of the study, led by Dr. Hee Young Lee, was to assess and compare multiplanar WBCT signs of first TMT joint instability between HV, HR, and control patients. In addition, they analyzed the first TMT joint morphology of the distal articular surface of the medial cuneiform (C1) The team hypothesized that signs of first TMT joint multiplanar instability would be found in HV and HR patients, and that specific anatomic variants of C1 would be more prevalent in the HV and HR group.
Materials and Methods
The study compared WBCT datasets from 27 HV patients, 26 HR patients, and 30 control patients. The WBCT scans were obtained via a CurveBeam pedCAT system. and analyzed in CubeVue, CurveBeam’s custom visualization software.
Four measurements were performed in the sagittal plane at the mediolateral center of the TMT joint. The inclination of the first TMT was defined as the angle between the longitudinal axis and the distal articular surface of C1. The first TMT joint angle was measured between the articular surfaces of C1 and M1 at the mediolateral center of the first TMT joint. The dorsal translation of M1 at the first TMT joint was defined as a step-off or discontinuation of the curvature along the plantar or dorsal borders of C1 and M1. To quantify dorsal translation of M1, plantar distance was defined as a vertical distance between the most inferior point of distal articular surface of C1 and proximal articular surface of M1 at the mediolateral center of the TMT joint.
In the axial plane, the inclination of the first TMT was measured at the dorsoplantar center of the first TMT joint. Thicker MPR slices were utilized to allow for measurements of four different angles including hallux valgus angle (HVA), first-second intermetatarsal angle (IMA), C1-M1 angle, and the middle cuneiform-second metatarsal angle (C2-M2). To determine varus angulation of proximal M1 (axial instability) at the first TMT joint, C1-M1 angle was defined as an angle between the longitudinal axes of C1 and M1. To determine forefoot adduction, simplified metatarsus adductus angle, C2—M2 angle was measured.
In the coronal plane, a total of four angulations were assessed: Rotational profile of the distal aspect of C1 and proximal aspect of M1 at the first TMT joint, rotational profile of the distal aspect of M1, and the forefoot arch angle. Distal C1 rotation and proximal M1 rotation angles were defined as angles between the vertical axes of C1 and M1 and the perpendicular line to the ground (pronation +/supination -). The vertical axes were drawn to connect midpoints of the interquartile lines of C1 and M1 just proximal and distal to the first TMT joint respectively. Rotational profile of the distal aspect of M1 (distal M1 rotation angle) was measured as an angle between a line connecting far points of the medial and lateral sesamoid sulcus and the floor line.
Conclusion
Results showed the HV group had significantly increased first TMT angle, IMA, C1-M1 angle, and rotational profile of the distal M1 compared with the control and HR groups. Dorsal translation of M1 was frequently found in the HV and HR groups with significantly increased plantar distance compared with the controls.
The results confirmed signs of first ray instability at the first TMT joint are often seen in both HV and HR patients. The HV group demonstrated instability mainly in sagittal and axial planes while the HR group predominantly had sagittal instability markers. There were no differences in C1 morphology when measured by the distal articular surface inclination, suggesting C1 morphology is not a predisposing factor for first ray instability development in either HV or HR. The results also validated previous studies, which found increased plantar gapping in HV and HR patients.
“A surgical stabilization of the instability at the first TMT joint can be an option for simultaneous correction of the first TMT angle, M1 dorsal translation in sagittal plane and increased C1-M1 angle, HVA, IMA in axial plane, and possibly proximal and distal M1 rotation in the coronal plane,” researchers found.
To read the full study please click here.