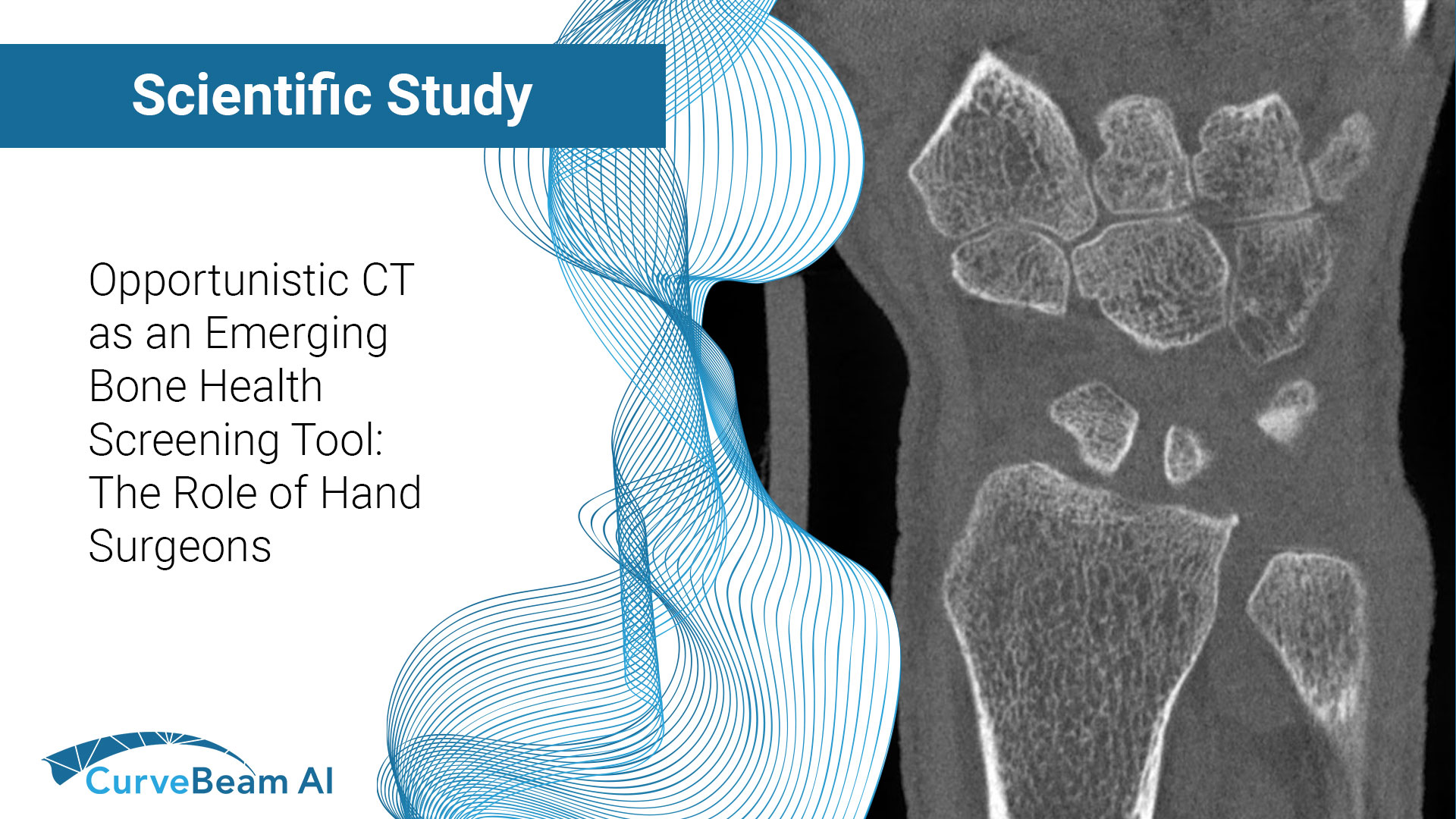
AI-Driven Segmentation on Weight Bearing CT Introduction Accurate segmentation is critical for orthopedic workflows, including…
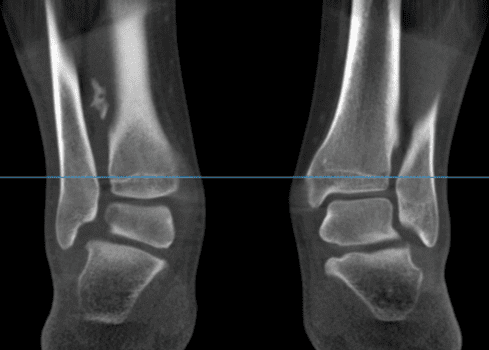
Lower Limb Influence on Hindfoot Alignment
A recent study headed by L. Baverel, a distinguished French M.D., came out of the European Foot and Ankle Society in 2016. The study, published in Elsevier, examines the effect lower limb placement, specifically rotation, has on hindfoot alignment.
The implications for the study are still being sorted through, but a few standouts are worth mentioning. This study points out a major problem with 2D radiographic assessments of hindfoot alignment: there are numerous factors that influence measurements. Rotation of the lower limb is the first and foremost of these factors. “In the near future, it is very likely that 3D, weight bearing CT technology will enable the development of new ways to measure hindfoot alignment, based on 3D hindfoot-forefoot divergence angles or offsets rather than tibia-calcaneus angles.”
The constant goal of all orthopedic surgeons is to facilitate the correct alignment of bones. Even the slightest error in measurement can have devastating consequences on post-surgery recovery and future mobility. As the study notes, “Abnormal coronal alignment of the hindfoot has been proven to increase the risk of degenerative pathology or surgical failure in the foot and ankle.” The results of this study bring us that much closer to understanding foot and ankle dynamics, and are already impacting X-ray, stabilization and recovery protocol around the world.
For the purposes of study, foot alignment depends on basic two-dimensional radiographic techniques. However, apart from two recent radiographic techniques, the Ground Reaction Force Calcaneal Offset (GRFCO) and Arunakul’s Tripod Index, all others depend on lower limb rotation. This is important, as lower limb rotation necessarily affects foot alignment. The study describes rotation as one of the variables explaining lack of reproducibility in assessing hindfoot alignment: “The hypothesis for this study was that a mathematical model predicts how [rotation] modifies radiographic hindfoot alignment measurements.”
The study concluded, “The mathematical model accurately predicted the variations of the hindfoot angle, which was maximum when the foot was aligned with the X-ray source. It then decreased when the foot rotated away, following a parabolic curve.” The Meary angle was at maximum value when incident X-rays were aligned according to the second metatarsal bone, then declined along a parabolic curve as the lower limb rotated away from this axis. The study plainly illustrates this dynamic at play. “In practical terms, during the Meary procedure for shooting an AP ankle view, misalignment of the foot (caused either by incorrect positioning of the patient or an actual deformity), results in underestimating the value of the hindfoot angle.”
Until 3D weight bearing CT is an available option, it is recommended foot & ankle specialists exercise caution when planning from 2D radiographs. Radiographic procedures must account for correct alignment of the foot. That means checking that the second metatarsal is aligned with the X-ray source. This procedure appears to most consistently approximate true alignment. If alignment isn’t based off that axis, the deformity could be underestimated and the radiography should be done again or carefully questioned. For more detail, access a link to the article here.